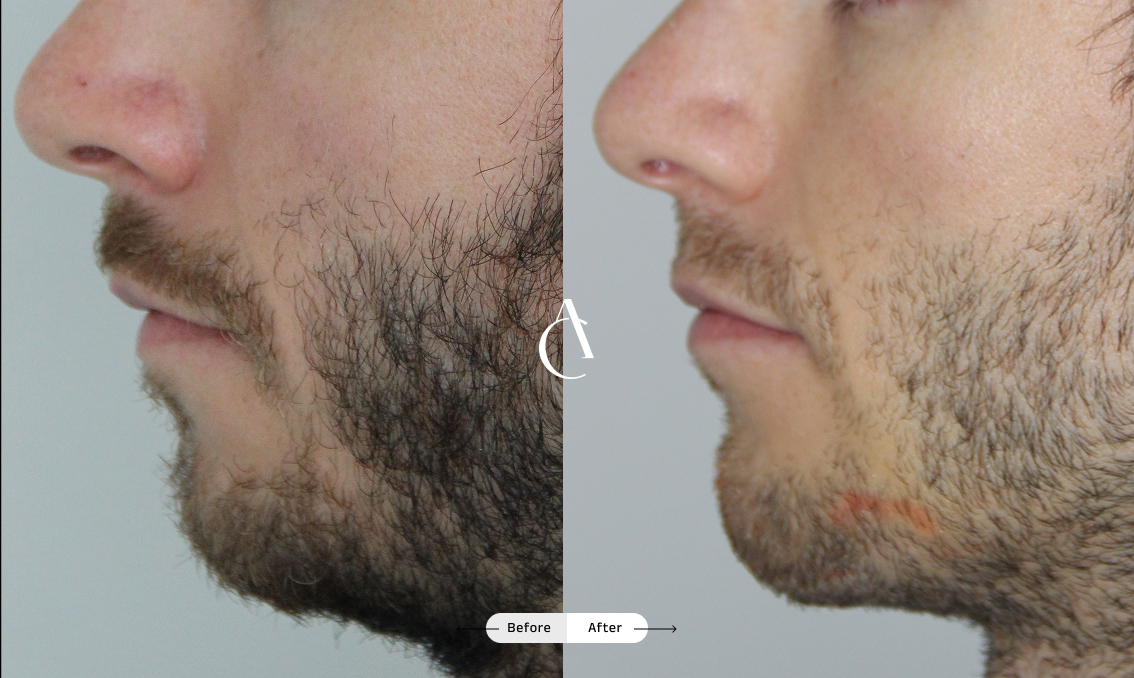
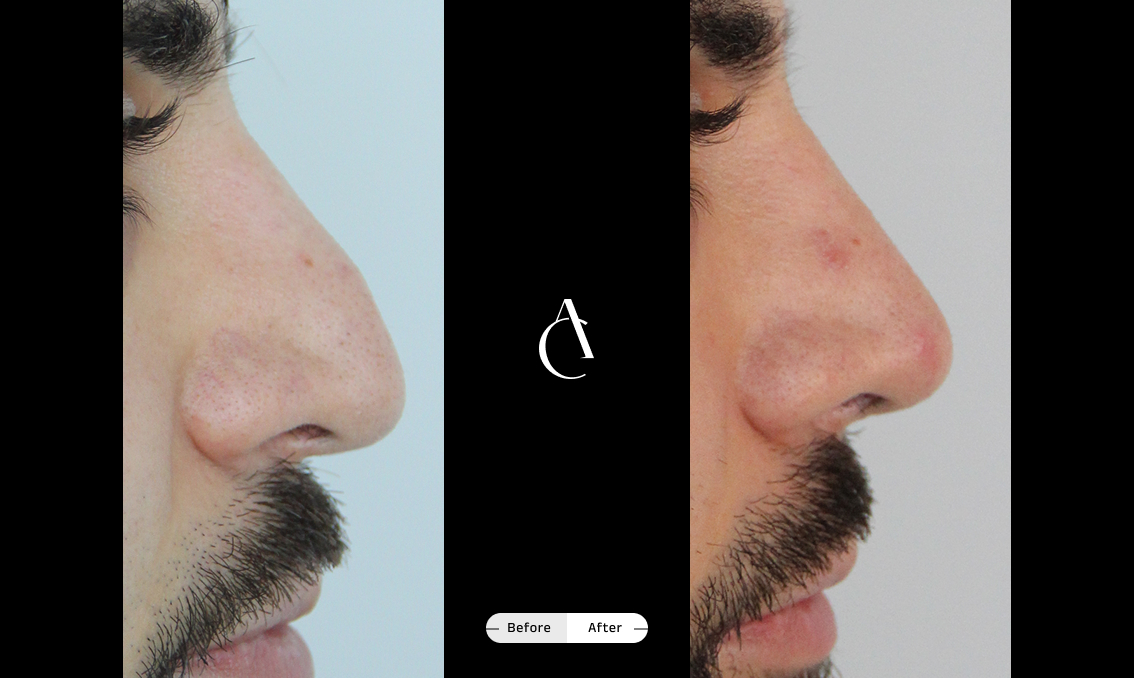
What is nasal obstruction and how does it affect breathing?
Nasal obstruction, sometimes called nasal blockage, refers to any condition that restricts airflow through your nose. This could be caused by structural issues, inflammation or a combination of both. People with narrow nasal passages or internal structural collapse often notice that their breathing feels laboured, especially when they’re sleeping or during physical activity.
Common symptoms include:
- Persistent stuffy or blocked nose
- Difficulty breathing through one or both nostrils
- Mouth breathing, particularly at night
- Snoring or disturbed sleep
- Reduced sense of smell
- Facial pressure or sinus discomfort
Over time, nasal obstruction can impact your energy levels, concentration and overall wellbeing. Athletes may find their endurance compromised, while others feel tired during the day from poor sleep quality.
Nasal obstruction treatment: what are the first steps?
Before considering surgery, most patients start with medical or lifestyle treatments aimed at reducing inflammation and improving airflow. These may include:
- Saline nasal rinses to clear mucus and allergens
- Steroid nasal sprays to reduce swelling
- Antihistamines or allergy management
- Treatment for sinus infections
- Adjusting sleeping position (for example, elevating your head)
- Weight management, where relevant – excess weight can make your breathing issues worse
For many people, these measures provide significant relief. However, when symptoms persist – particularly if you have structural problems in your nose – surgery may be recommended to address the underlying cause rather than just your symptoms.
Common causes of nasal blockage requiring surgery
Several anatomical and medical conditions can lead to persistent blockage of your nose, and identifying the cause of your symptoms is key to choosing the right treatment. Common root problems include:
- Deviated septum: a displacement of the wall dividing your two nasal passages that narrows one side and restricts airflow.
- Enlarged turbinates: swollen structures inside your nose that can obstruct your breathing. These are often linked to allergies or chronic inflammation.
- Narrow nasal passages and valve collapse: weak or narrow areas that limit airflow, especially during deep breathing. This often requires specialised narrow nasal passages treatment.
- Nasal polyps or chronic sinusitis: soft growths or long-term inflammation that block airflow and contribute to congestion.
- Trauma or previous surgery: injury or earlier procedures may alter your nasal structure, sometimes requiring nasal blockage removal surgery to restore function.
You may have more than one of these factors involved, which is why your treatment plan will be tailored to you.

Images source: Envato
Nasal surgery for breathing: what procedures are available?
There are several types of nasal surgery designed to improve your breathing, and the right procedure (or combination) for you will depend on the cause of your obstruction.
Septoplasty
This straightens a deviated septum to open your nasal airway, and it’s one of the most common procedures for nasal obstruction.
Turbinate reduction
This reduces the size of enlarged turbinates to create more space for airflow while preserving their important function.
Nasal valve surgery
This strengthens or widens the narrowest part of your nasal airway, and it’s particularly helpful for patients with valve collapse.
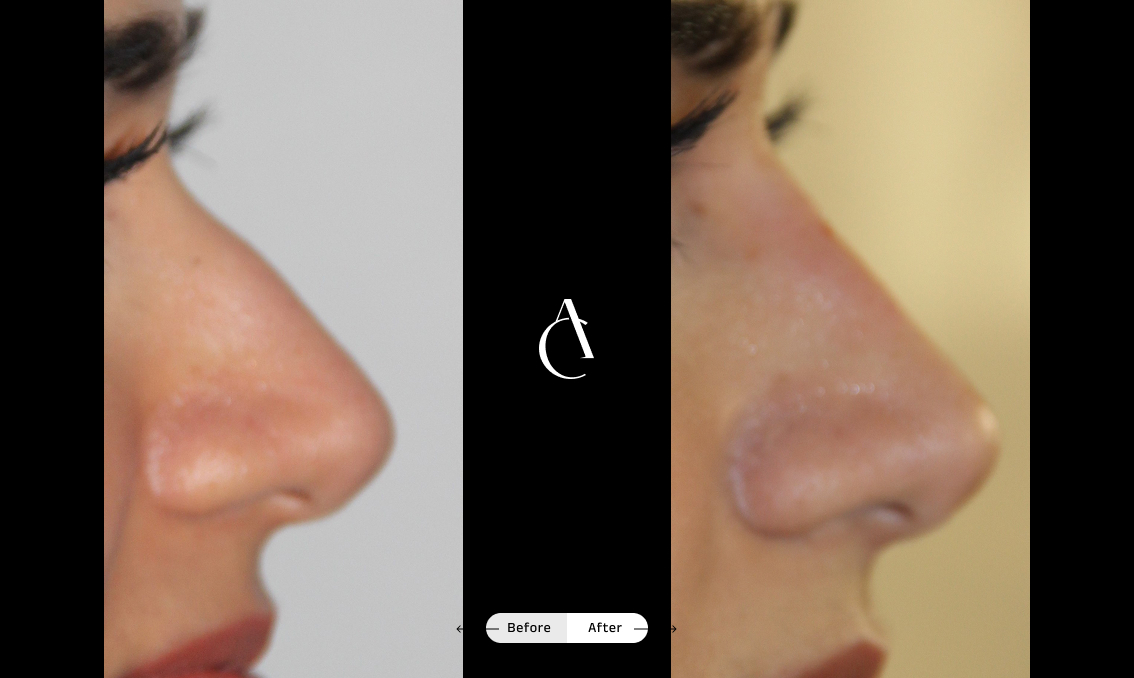
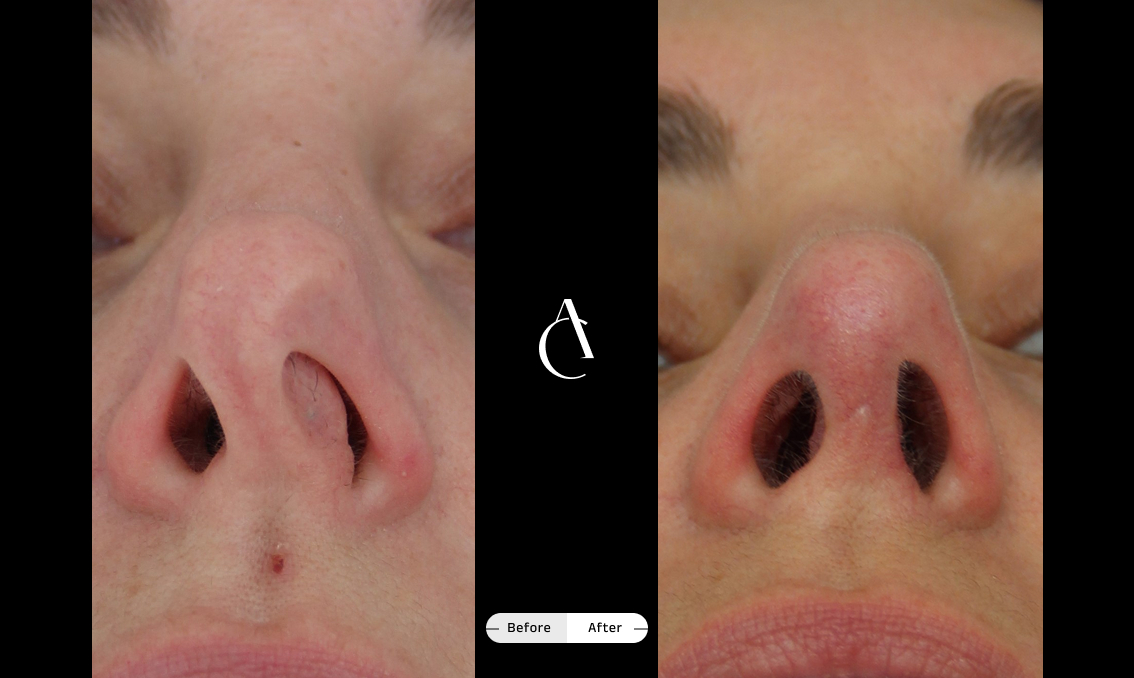
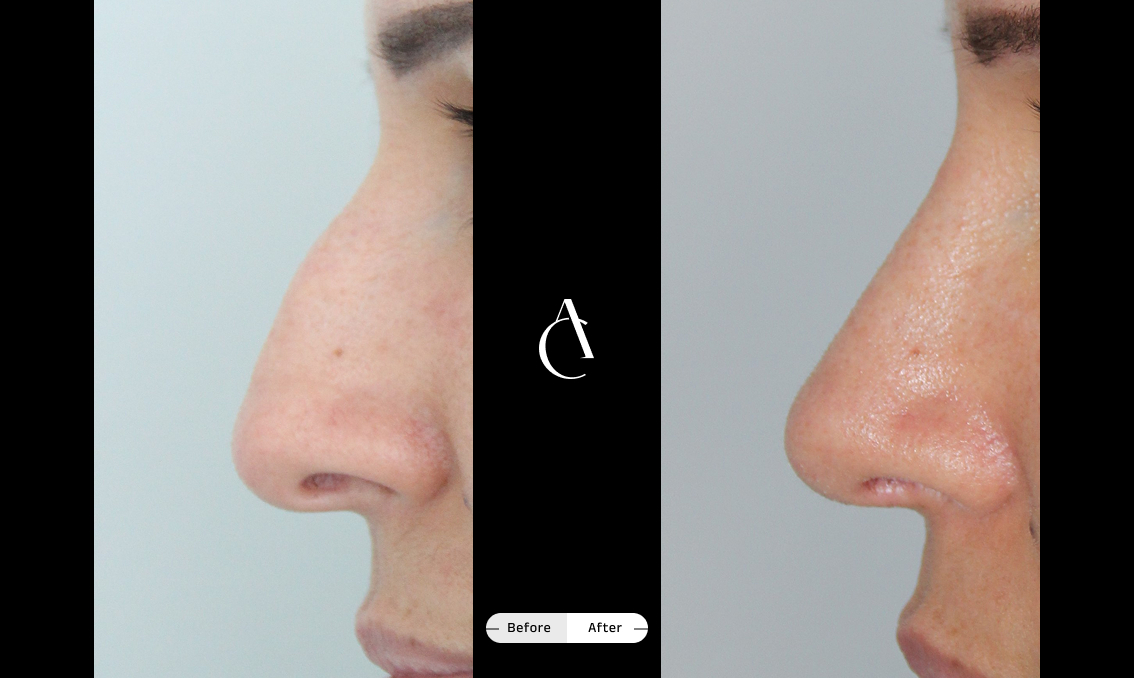
Functional rhinoplasty
Functional rhinoplasty addresses structural issues affecting your breathing, such as weak cartilage or external deformities, and may also refine the appearance of your nose if needed or desired.
Surgeons often combine these techniques to achieve the most durable result.
What to expect before and after nasal obstruction surgery
Before your surgery, you’ll undergo a detailed pre-operative assessment that may include:
- A consultation to discuss your symptoms and medical history
- An examination of your nose and endoscopy
- Imaging such as CT scans if sinus disease is suspected
- A breathing assessment
Your surgeon will explain the planned procedure, expected benefits and recovery timeline. After surgery, it’s normal to experience:
- Temporary swelling and congestion
- Mild discomfort or pressure
- A feeling of blockage while tissues heal
Most people notice breathing improvements within a few weeks as swelling subsides, although full healing can take longer depending on the complexity of the procedure you’ve undergone.
Most patients can return to work around a week after surgery and resume light activity after two weeks. It’s best to wait at least three or four weeks and seek your surgeon’s approval before strenuous exercise. Be sure to attend any follow-up consultations to ensure your healing is progressing well and to help optimise your results.
Images source: Envato
Benefits and risks of nasal obstruction surgery
Like any medical procedure, nasal obstruction surgery has both benefits and potential risks. Benefits may include:
- Better nasal airflow and easier breathing
- Better sleep and less snoring
- Better exercise performance
- Fewer sinus infections
- Reduced reliance on medications
Possible risks include:
- Bleeding or infection
- Persistent or recurrent blockage
- Temporary changes in sensation
- Some cases may need revision surgery
Choosing an experienced surgeon like Dr. Cuno and carefully following post-operative advice helps minimise these risks.
Is nasal obstruction surgery right for you?
You may wish to consider surgery if your nasal blockage is persistent or worsening, if medical treatments haven’t given you sufficient relief and if your breathing difficulties are affecting your sleep, work or daily activities. It’s also worth looking into if you experience frequent sinus problems or mouth breathing, or if you have structural issues such as a deviated septum or valve collapse.
Book a consultation with Dr. Cuno at his Geneva clinic to explore your options and find out how treatment could improve both your breathing and quality of life.