Is it normal to have breathing problems after rhinoplasty?
Temporary breathing difficulties are very common after rhinoplasty. In the first days and weeks after your surgery, your nose will be swollen internally, and many patients report feeling blocked or congested. Typical sensations include:
- Needing to breathe through your mouth, especially at night
- A feeling of pressure or fullness inside your nose
- Mild blockage on one or both sides
- Crusting or dried secretions
- Reduced airflow compared to before surgery
Internal swelling, healing tissues and sometimes splints or packing can all contribute to these symptoms, but most patients notice a gradual improvement as their nose heals.
Remember, recovery varies. Some people feel clearer sooner, while others take longer, particularly after complex or revision procedures.
Main causes of breathing problems after rhinoplasty
Breathing changes can be caused by several factors, some temporary and others structural. These include:
- Post-operative swelling and internal splints: swelling narrows the airways, while splints can temporarily restrict airflow.
- Crusting, dried blood and mucus: the normal healing process produces debris that may block your nasal passages until they’re gently cleansed or it’s dissolved with saline.
- Narrowing of the nasal valve or over-resection of cartilage: if structural support is reduced, airflow resistance may increase.
- Septal deviation or perforation: occasionally, your septum may heal unevenly or develop a small hole that affects airflow.
- Pre-existing sinus or allergy issues: any underlying conditions you have may become more noticeable during recovery.
Most causes are temporary, but structural problems require careful evaluation.
How long do breathing problems last after rhinoplasty?
It’s worth taking the time to understand how rhinoplasty recovery normally progresses so that you know what to expect. Here’s a typical timeline.
- First 1-2 weeks: congestion is at its peak. Mouth breathing and a blocked nose sensation are common, especially while your splints are in place or swelling is pronounced.
- Weeks 3-6: nasal airflow usually improves gradually as the swelling goes down and your internal nasal tissues settle.
- Several months: subtle improvements continue as deeper swelling subsides and scar tissue matures.
While mild obstruction can persist for a while, severe or worsening blockage is not normal and you should discuss it with your surgeon as soon as possible.
Read more about rhinoplasty recovery.

Images source: Envato
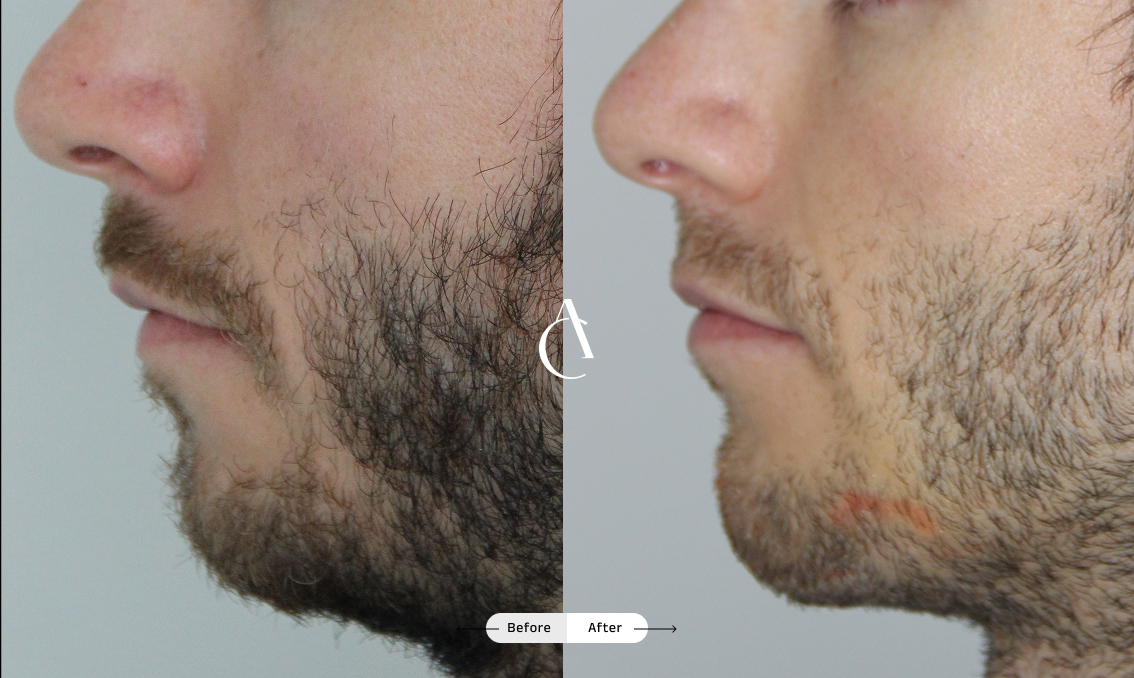
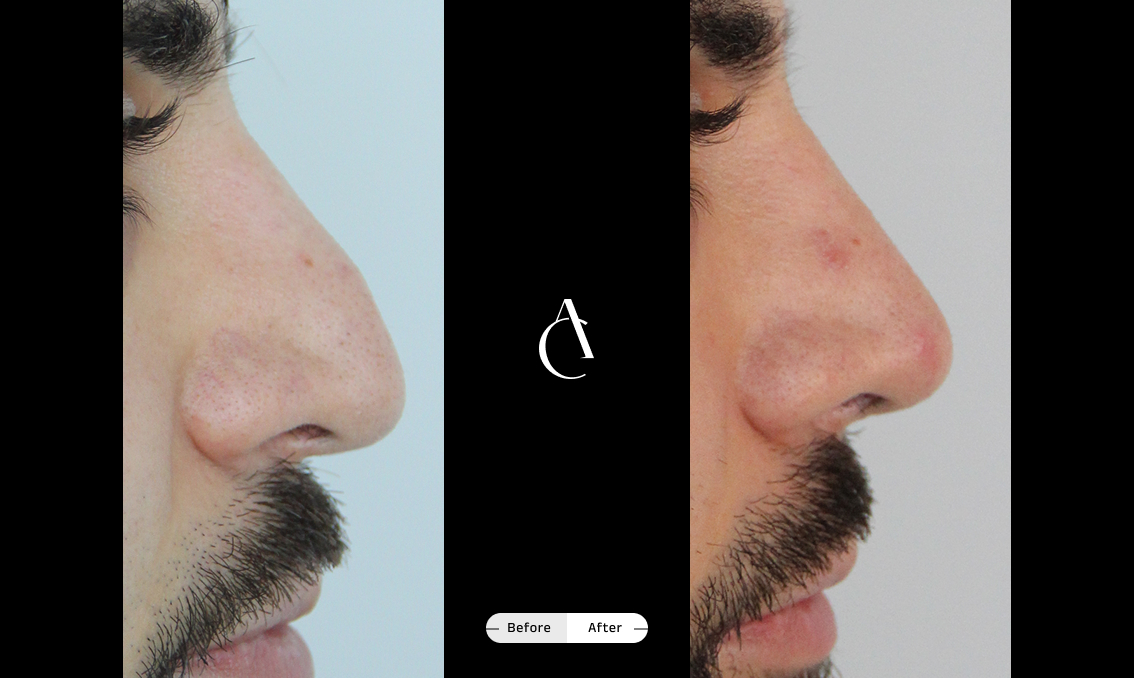
Rhinoplasty to correct breathing problems
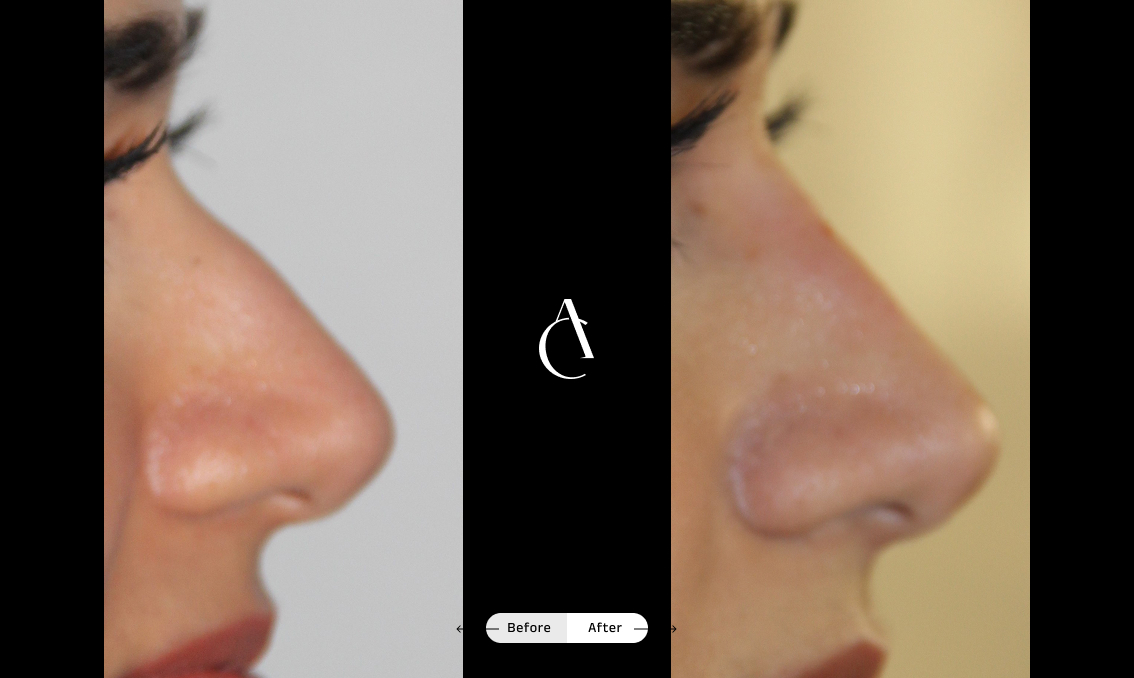
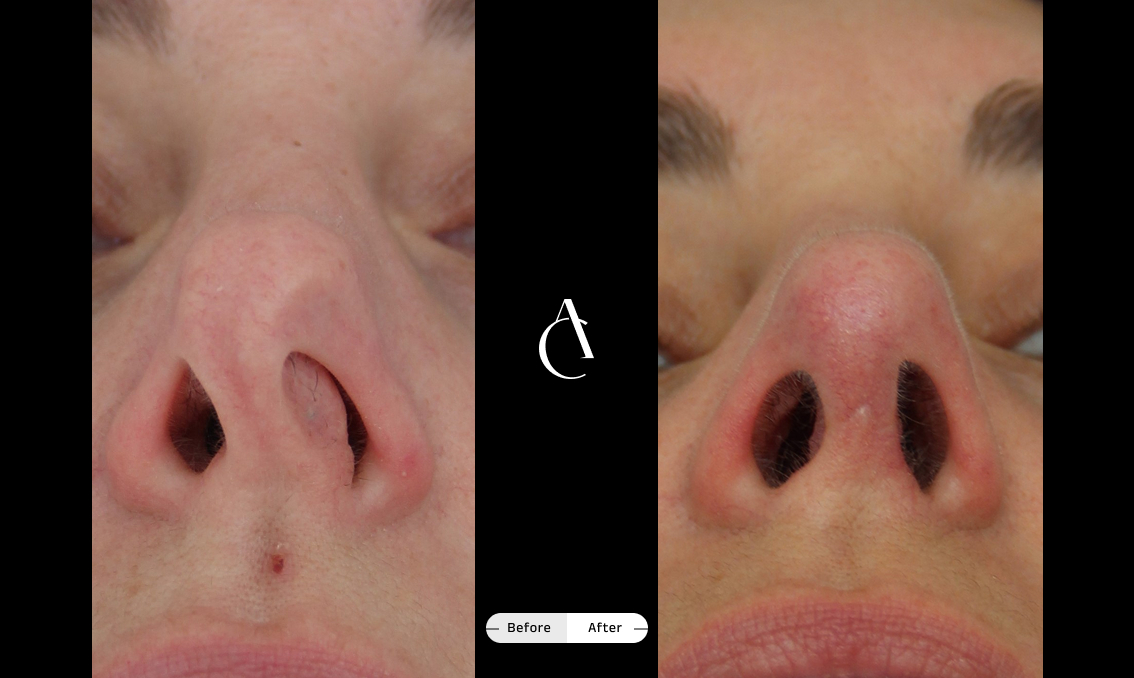
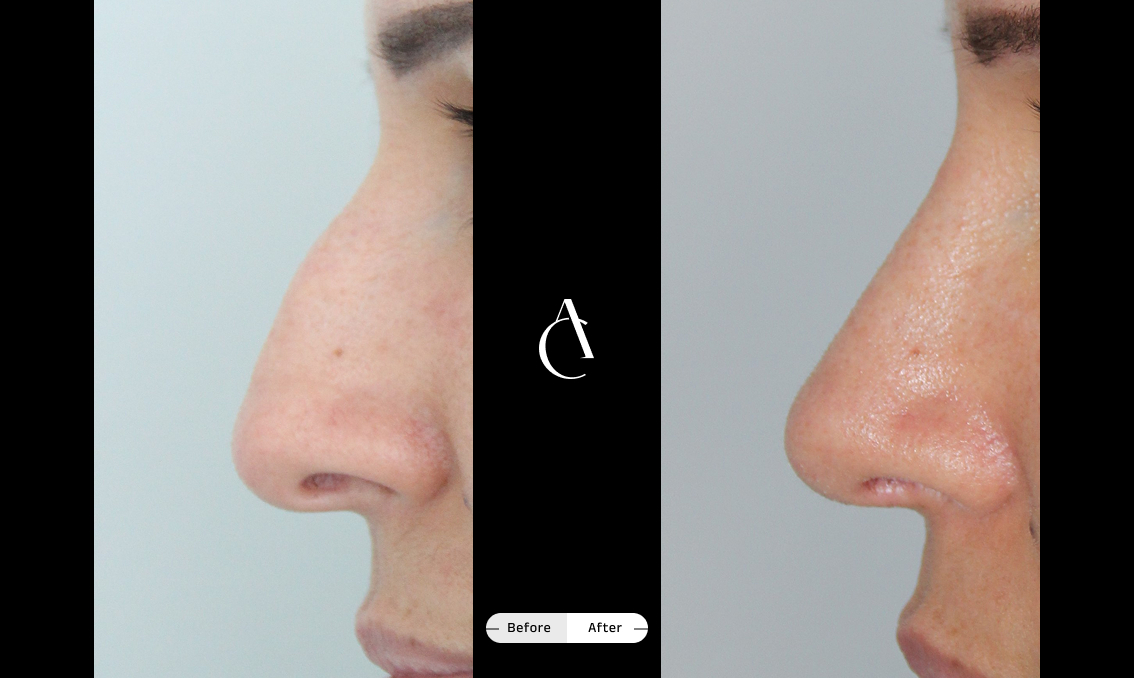
Rhinoplasty isn’t just about improving the appearance of your nose; it can also be used to correct asymmetry, improve nasal function and help you breathe more easily. A functional rhinoplasty procedure can address structural issues in your nose that are causing the obstruction.
If you’re seeking rhinoplasty for breathing problems and asymmetry, talk to your surgeon about the available techniques to strengthen weak nasal valves, straighten a deviated septum, correct a crooked or collapsed nose or simply improve symmetry and airflow.
When should you worry about breathing problems after rhinoplasty?
While temporary congestion is normal, certain symptoms may indicate a problem. Contact your surgeon immediately if you experience any of the following red flags:
- Painful obstruction on one side of your nose
- Persistent inability to breathe through your nose after several weeks
- Whistling sounds, marked asymmetry or visible collapse when breathing in
- Fever, foul odour or discharge – this suggests infection
- Sudden worsening after initial improvement

Images source: Envato
How to ease breathing problems during rhinoplasty recovery
There are several simple ways to make your recovery more comfortable and support healing:
- Use saline sprays or rinses as recommended by your surgeon to keep your nose moist and clear of debris
- Sleep with your head elevated to reduce swelling
- Avoid blowing your nose or strenuous activity during early recovery
- Use a humidifier or gentle steam to prevent dryness
- Avoid smoky or dusty environments
It’s important not to use over-the-counter decongestant sprays unless your surgeon advises, as they can irritate healing tissues or cause rebound congestion.
When is revision or functional rhinoplasty needed for breathing problems?
In some cases, breathing issues persist due to structural changes such as valve collapse, scar tissue or unresolved septal problems. Your surgeon may recommend a secondary procedure, often called revision rhinoplasty, or a septorhinoplasty. Revision surgery is usually considered after 9 to 12 months, once healing stabilises, and the goal is to restore airflow while preserving or improving the shape of your nose.
Careful planning of this kind of surgery is essential, as revision procedures are more complex. Surgeons who are experienced in both functional and aesthetic nasal surgery, such as Dr. Cuno, are well placed to assess complex breathing concerns and develop solutions tailored to your own anatomy and issues.
Breathing problems after rhinoplasty and how to address them
Rhinoplasty can both cause and correct breathing problems, and changes to airflow are common after rhinoplasty – particularly in the early healing phase. Most patients experience temporary congestion that improves steadily over time, so it’s important to monitor your symptoms and attend follow-up consultations when you’re invited. Severe or persistent blockage isn’t normal, and if this happens you should contact your surgeon immediately.
If you’re experiencing on-going breathing difficulties or you’d like reassurance about your recovery, consider booking a consultation with Dr. Cuno to review your symptoms and discuss the best next steps.